Insurance verification is one of the most important responsibilities handled by the front desk in UAE clinics. A single mistake during eligibility checks or patient registration can lead to rejected claims, delayed payments, patient complaints, compliance issues, and revenue leakage.
In many clinics across the UAE, receptionists are the first point of contact for insured patients. They are responsible for collecting insurance details, checking eligibility, confirming coverage, and ensuring the patient profile is correctly updated before the consultation begins. While this process may appear simple, it directly affects claim acceptance rates, patient satisfaction, and clinic cash flow.
With healthcare authorities in the UAE increasingly focusing on standardized insurance workflows, clinics must properly train front desk teams to handle insurance verification professionally and consistently. Platforms such as eClaimLink and the Riayati e-Claims Post Office now play a major role in insurance eligibility checks, claims exchange, authorization workflows, and payer-provider communication in the UAE healthcare ecosystem.
This guide explains how UAE clinics can properly train their reception and front desk teams on insurance verification procedures, workflows, compliance standards, and patient communication.

Why Insurance Verification Matters in UAE Clinics
Insurance verification is not just an administrative task. It is a revenue protection process.
When insurance details are entered incorrectly or eligibility is not checked properly, clinics may face:
- Claim denials
- Delayed reimbursements
- Incorrect patient billing
- Compliance violations
- Authorization rejections
- Patient dissatisfaction
- Increased front-office workload
- Revenue loss
In the UAE healthcare system, insurers, TPAs, healthcare providers, and government health authorities rely heavily on electronic claim systems and standardized data exchange. Platforms such as eClaimLink and Riayati support real-time insurance workflows between healthcare providers and payers. These include eligibility checks, authorizations, claim submissions, and insurance response exchanges.
This means front desk staff must understand that insurance verification is not optional or “just reception work.” It is a critical operational function that impacts the entire clinic.
Understanding the UAE Insurance Verification Workflow
Before training staff, clinic management should ensure every receptionist understands the full insurance journey of a patient.
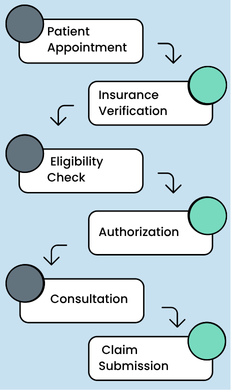
A standard UAE insurance verification workflow usually looks like this:
1. Appointment Booking
When the patient calls or books online, the receptionist asks:
- Is the visit insurance or cash?
- Which insurance company is the patient using?
- Is the patient visiting for the first time?
- Is the Emirates ID available?
At this stage, many clinics already perform preliminary eligibility checks.
2. Patient Arrival
When the patient arrives:
- Emirates ID is collected
- Insurance card is collected
- Patient information is verified
- Insurance details are added to the patient profile
The receptionist then opens the insurance portal or integrated clinic software to check eligibility.
The receptionist enters patient details such as:
- Emirates ID number
- Member ID
- Insurance card number
- Date of birth
- Insurance provider
The portal then confirms:
- Active policy status
- Coverage validity
- Network eligibility
- Co-payment rules
- Exclusions
- Approval requirements
4. Consultation and Authorization
If authorization is required:
- Medical details are submitted
- Insurance approval is requested
- The payer responds electronically
5. Claim Submission
After treatment:
- Claims are prepared
- Coding is validated
- Claims are submitted electronically
Platforms such as Riayati and eClaimLink support these insurance workflows in the UAE.
Train Front Desk Staff on UAE Insurance Basics
Many receptionists know how to “check insurance,” but they do not actually understand insurance structures. Training should start with insurance fundamentals. Reception staff should understand:
- Difference between insurance companies and TPAs
- Basic vs enhanced plans
- In-network vs out-of-network coverage
- Co-payments and deductibles
- Pre-authorization requirements
- Policy exclusions
- Expiry dates
- Annual limits
- Coverage categories
For example, some UAE patients may assume all clinics are covered under their insurance plan, but network restrictions may apply. Receptionists must know how to identify these issues before consultation begins. This prevents disputes at checkout and protects the clinic from rejected claims.
Train Staff on Insurance Portals and Systems

One of the biggest challenges in UAE clinics is inconsistent portal usage among front desk teams. Some staff may know only one insurer portal, while others rely entirely on verbal confirmation from patients. This creates major operational risks.
Receptionists should be trained to properly use:
- Insurance portals
- TPA portals
- Eligibility verification tools
- Integrated clinic management systems
- eClaimLink workflows
- Riayati-related insurance exchanges
The Riayati e-Claims Post Office enables providers to exchange eligibility requests, authorization requests, claims, and payer responses through a unified digital platform.
Similarly, eClaimLink provides standardized datasets, payer lists, coding guidelines, provider workflows, and insurance exchange support in Dubai.
Front desk staff should understand:
- How to log into portals securely
- How to search patients correctly
- How to interpret eligibility results
- How to identify inactive policies
- How to identify network mismatches
- How to document verification evidence
Create a Standardized Verification Checklist
Every clinic should create a fixed insurance verification checklist. Without standardization, every receptionist develops their own process, leading to errors and inconsistency. An ideal insurance verification checklist includes:
Patient Identity Verification
- Confirm Emirates ID
- Confirm patient mobile number
- Verify date of birth
Insurance Verification
- Check insurance card validity
- Verify policy activation
- Confirm network eligibility
- Confirm consultation coverage
- Check co-pay percentage
- Review exclusions if applicable
Documentation
- Upload insurance card copy
- Upload Emirates ID copy
- Update patient profile
- Save eligibility response
Financial Confirmation
- Inform patient of co-pay amount
- Explain non-covered services
- Confirm approval requirements
Front desk teams should use the same workflow for every patient. Consistency reduces claim denials significantly.
Teach Staff How to Handle Eligibility Responses Properly
A major problem in clinics is that staff only check whether insurance is “active.” That is not enough. Receptionists must learn how to interpret eligibility results carefully.
Eligibility responses may indicate:
- Coverage active
- Coverage expired
- Provider not in network
- Referral required
- Authorization required
- Service excluded
- Policy suspended
Front desk employees should never assume that “active insurance” means “fully covered.” Proper training should include real examples and simulations.
Train Receptionists on Patient Communication
Insurance conversations can become stressful. Patients may become frustrated if coverage is denied or co-payments are higher than expected. Reception staff should be trained to communicate professionally and clearly.
Important communication principles include:
- Never promise approval before verification
- Never guess insurance coverage
- Explain co-payments politely
- Use simple language
- Avoid blaming insurers aggressively
- Escalate complex issues to billing teams
For example:
Instead of saying:
“Your insurance is rejected.”
Receptionists should say:
“Your insurance eligibility is currently showing as inactive in the payer system. Let me double-check the details for you.”
This reduces tension and improves patient trust.
Use Real-Life Scenarios During Training
One of the best training methods is scenario-based learning. Instead of only giving theoretical instructions, clinics should simulate real insurance situations. Examples include:
Scenario 1: Expired Insurance
Patient arrives with expired coverage. Receptionist should:
- Verify expiry date
- Inform patient professionally
- Offer cash consultation option
Scenario 2: Wrong Network
Patient insurance active but clinic not covered. Receptionist should:
- Explain network restriction
- Verify if reimbursement is possible
- Inform patient before consultation
Scenario 3: Authorization Required
Patient requires MRI approval. Receptionist should:
- Inform patient about authorization timeline
- Coordinate with insurance coordinator
- Avoid promising immediate approval
This type of practical training improves confidence significantly.
Train Staff on Documentation Accuracy
Insurance verification is highly dependent on accurate patient data. Even small mistakes can cause claim rejections.
Common front desk errors include:
- Wrong Emirates ID number
- Incorrect member ID
- Misspelled patient names
- Wrong payer selection
- Missing insurance card uploads
- Duplicate patient profiles
Receptionists should understand that inaccurate data affects:
- Eligibility checks
- Authorizations
- Claims processing
- Reimbursements
- Compliance audits
Healthcare data quality is becoming increasingly important in UAE healthcare integrations and centralized systems. Discussions around UAE healthcare interoperability platforms frequently highlight challenges involving incomplete or inaccurate patient information.
Explain the Importance of Compliance
Insurance verification is also a compliance issue. UAE healthcare authorities expect providers to maintain proper insurance documentation and accurate electronic records.
Systems such as eClaimLink standardize healthcare insurance data exchange and coding requirements in Dubai.
Receptionists should understand:
- Why eligibility must be checked before treatment
- Why insurance cards must be uploaded
- Why patient consent matters
- Why documentation must be complete
- Why audit trails are important
Staff should never bypass workflows “to save time.
Build Coordination Between Front Desk and Billing Teams
Insurance verification should not operate independently from billing and claims departments.
Front desk teams should coordinate closely with:
- Insurance coordinators
- Medical coders
- Billing staff
- Claims departments
Regular communication helps identify recurring issues such as:
- Specific insurers rejecting claims
- Frequent eligibility mismatches
- Missing authorization patterns
- Incorrect patient registrations
This creates continuous improvement across the clinic.
Monitor Front Desk Insurance KPIs
Training alone is not enough. Clinic management should measure insurance verification performance regularly.
Useful KPIs include:
- Eligibility verification accuracy rate
- Claim rejection percentage
- Registration error rate
- Average patient check-in time
- Authorization turnaround time
- Front desk productivity
- Insurance-related patient complaints
Tracking these metrics helps clinics identify weaknesses early.

Conduct Refresher Training Regularly
Insurance workflows in the UAE change frequently. New payer rules, coding updates, network changes, and compliance requirements are introduced regularly.
The eClaimLink portal continuously updates payer lists, coding datasets, circulars, and technical requirements. Front desk staff should receive refresher training every few months.
Topics should include:
- New insurance policies
- Updated workflows
- Common rejection reasons
- Patient communication improvements
- System updates
- Data accuracy improvements
Common Insurance Verification Mistakes UAE Clinics Should Avoid
Many UAE clinics repeatedly face the same front desk problems.
Skipping Eligibility Checks:
Some receptionists assume returning patients still have active insurance. Policies can expire or change unexpectedly.
Relying Only on the Insurance Card:
An insurance card alone is not proof of active coverage. Eligibility must always be verified electronically.
Incorrect Data Entry:
Even one incorrect digit in the Emirates ID can affect claim processing.
Poor Documentation:
Missing insurance uploads and incomplete patient files can lead to audits and claim denials.
Promising Coverage Too Early:
Receptionists should never guarantee insurance approval before verification.
The Role of Technology in Insurance Verification
Modern clinic software significantly improves front desk insurance workflows.
Integrated systems help automate:
- Eligibility checks
- Patient registration
- Insurance validation
- Authorization tracking
- Claims preparation
- Document uploads
When front desk systems integrate with payer workflows and healthcare exchange systems, clinics reduce manual errors and improve efficiency.
This is especially important as UAE healthcare continues moving toward connected digital ecosystems involving platforms like Riayati and eClaimLink.
How Proper Training Improves Patient Experience
Insurance problems are one of the biggest causes of patient frustration in UAE clinics. Online discussions frequently show patients complaining about claim rejections, coverage confusion, insurer delays, and conflicting eligibility information.
A properly trained front desk team helps prevent these situations by:
- Verifying coverage accurately
- Explaining policies clearly
- Reducing waiting times
- Preventing billing surprises
- Improving communication
- Managing expectations early
Patients trust clinics more when insurance handling is smooth and professional.
Create Written SOPs for Front Desk Insurance Verification
Every clinic should document its insurance workflow formally. A proper SOP should include:
- Appointment verification process
- Required patient documents
- Portal login procedures
- Eligibility verification steps
- Escalation procedures
- Authorization workflows
- Cash conversion policies
- Documentation standards
Written SOPs make onboarding easier and reduce operational inconsistency.
Train New Staff Before Independent Access
New receptionists should never immediately receive full insurance responsibilities without supervision. A proper onboarding process includes:
Phase 1: Observation
New staff observe experienced receptionists.
Phase 2: Guided Practice
They perform eligibility checks under supervision.
Phase 3: Independent Verification
They handle cases independently while being audited. This reduces costly errors during onboarding.
Encourage Accountability at the Front Desk
Receptionists should understand that insurance verification affects the clinic financially. When employees feel disconnected from claim outcomes, verification quality often drops. Management should share metrics such as:
- Claim rejection rates
- Revenue losses from incorrect verification
- Authorization delays
- Patient complaint trends
This creates ownership and accountability.
How Balsam Medico Can Help UAE Clinics
Managing insurance verification manually can become overwhelming for growing clinics. An integrated clinic management system can help front desk teams streamline:
- Patient registration
- Insurance verification
- Eligibility workflows
- Appointment management
- Insurance documentation
- Claims preparation
- Audit tracking
For UAE clinics handling multiple insurers and TPAs, automation reduces administrative burden while improving accuracy and compliance.
Solutions like Balsam Medico help clinics standardize workflows, reduce front-office errors, and improve coordination between reception, billing, and insurance teams.
By centralizing insurance-related operations, clinics can improve reimbursement efficiency while delivering a smoother patient experience.
Final Thoughts
Insurance verification is one of the most important operational responsibilities inside UAE clinics. A well-trained front desk team protects clinic revenue, improves patient satisfaction, reduces claim rejections, and supports compliance requirements.
As UAE healthcare systems continue moving toward greater digital integration through platforms such as Riayati and eClaimLink, clinics must ensure reception teams understand modern insurance workflows properly.
The most successful clinics treat insurance verification as a structured operational process rather than a basic administrative task.
By investing in training, standardization, communication, and technology, clinics can build a front desk team that handles insurance verification accurately, professionally, and efficiently every day.

Connect with Us
Ready to embark on this exciting journey? Contact us today:
📍 Dubai, United Arab Emirates – Tel: +971 56 640 9602
📍 Khartoum, Sudan – Tel: +249 91 273 1048
Explore Balsam Medico and discover a world of efficient clinic management at www.balsammedico.com. Together, let’s reduce fines, elevate efficiency, and embrace a new era of dental healthcare.
Join the Balsam Medico newsletter for exclusive content and the latest news. Be the first to view valuable information and updates!
